(I don’t want to bore you with my credentials, so if you want to see why I think I am qualified to criticize this website scroll to the bottom of this article.)
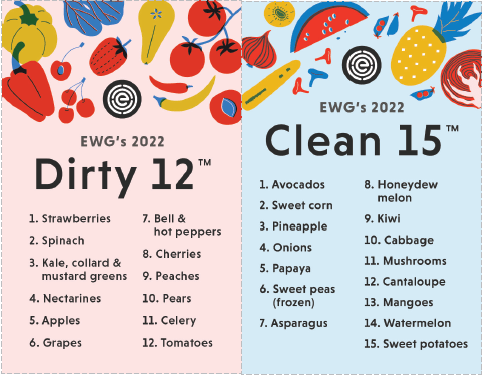
I recently came upon the 2022 version of the Environmental Working Group’s Dirty Dozen. This is a yearly posting from this group that alerts the public to the dozen fruits or vegetables that the EWG considers most highly contaminated with pesticides and for which the public should consider avoiding or considering organic alternatives. I have had several concerns about this list for a number of years and would now like to explain those concerns. In a word, there is a misconception of the analytical chemistry, the toxicology, and the nutrition of these 12 healthy foods. If you bear with me then I will explain some of the problems I see with this posting and why eating as many fruits and veggies as you can get your hands on is good for you.
Let me start with a famous maxim from Paracelsus, a sixteenth century quack, polymath, and “father of toxicology”. “Sola dosis facit venenum” or famously “Only the dose makes the poison”. As we review the Dirty Dozen and the data that supports them, it will be important to remember that anything can be a poison if the dose is high enough and anything can be relatively safe if the dose is low enough.
First though, let me start with an overview of what the Dirty Dozen are and who the EWG is. In a word, the EWG is about pesticides and other chemicals in our environment and protecting us from them by direct communication with consumers and by shining “a spotlight on outdated legislation, harmful agricultural practices and industry loopholes that pose a risk to our health and the health of our environment.” They have been publishing the Dirty Dozen since 2004. Each year the list varies a little and each year major news organizations cover the new list and suggest ways to avoid these foods. As you can well imagine, certain industry groups are not happy about this list and put out their own statements downplaying the dire warning of the EWG.
The Dirty Dozen report contains several positive aspects that I would be remiss in not mentioning. First, they use good clean government data from the USDA and the FDA in their computation and assessment. They are not so far on the fringe as to concoct myths from whole cloth. Second, in their report, which regrettably few people will read, they do tell their readers, “A critical part of a healthy diet includes a combination of fruits and vegetables, regardless of how they are grown.” While I will take issue with some of their other statements in a minute, we can both agree on this. More fruits and veggies are good for you, regardless of how they are grown.

So now let’s get into the weeds, looking at the numbers and the toxicology. (Analytical Chemistry and Nutrition next week.) The USDA does not assess every commodity every year so I went to a fruit that I was familiar with and that is near to the top of the Dirty Dozen every year, apples. Any citizen can find these data. Go to the Pesticide Data Program of the USDA. On the left you will find the PDP Database Search. For Apples, you will click on Apples, “Click All Pesticides” and “2016” from the Year column. From the Output Preference pull down menu and select “Summary of Findings” and “Search”. Wait a minute for the search and you should have 201 pesticides listed that were tested in 531 apple samples tested in 2016. Amazing. I have attached that spreadsheet below, so you don’t have to download it. The USDA samples the way that a consumer would. They go to stores and growers, obtain random samples of apples from all over the country, rinse them off the way a consumer should and prepare them the way a consumer would. In some cases that would involve peeling. On the table, notice how many samples had “defects”, meaning they tested positive for a pesticide. I counted 47 different positive pesticide defects. EWG generously only counts those with 2 or more positives. That lowers our count to 39. Of course, not every pesticide was found in every apple. On average there were about 4 “defects” per apple sample.

Let’s look at the details. There are some interesting stories here. In the EPA Tolerance column notice the “NT” values. These are “No Tolerance” pesticides, meaning that the EPA does not want to see any of these chemicals. These are basically outdated bad chemicals that have been banned or regulated. So how did our American farmers do with the nasties? Notice that there is not a single “defect” for an NT chemical in the list. American apple farmers are completely clean at the undetectable level for the baddest of baddies. It is a bit sad that the EWG did not brag about this. But no, apples are on the Dirty Dozen.
Now let’s compare the EPA Tolerance level with the Max detect column. This compares the highest level of each pesticide found and compares it with the highest level that the EPA allows. If the Max is higher than the EPA Tolerance, then someone has broken the rules. Since we have so many to compare, I created another column that takes the ratio of the two: max/Tolerance. If it is >1.0 then there is a violation. But the highest value in that column is 0.66 for the fungicide Thiabendazole. I call that “not bad” for 201 pesticide residues in 531 apples from all across the US. In fairness, the EWG will argue that some of those tolerances should be lower, but across the board, things look pretty safe. In fact, the average ratio of max to tolerance is 10%, meaning that of the residues found, the most extreme value of each is on average about an order of magnitude below the tolerated amount. Again, pretty safe.
Let’s go to the other extreme and look at the chemicals that show up in a large number of samples, over 20%. Most of them are fungicides: Thiabendazole, Pyrimethanil, Pyraclostrobin, Fludioxonil, and Boscalid. Two are insecticides: Chlorantraniliprole and Acetamiprid (a neonicotinoid insecticide). One is a post-harvest preservative that acts as an antioxidant and fungicide, Diphenylamine. So, what about these common chemicals? Here is what I know about growing apples. Humans love to eat apples. We each eat about 10 pounds a year. But do you know what loves to eat apples even more? Fungus and insects! It is an absolute war out there. Apple growers must spray something, usually a fungicide of one kind or another or an insecticide every two weeks all season long on their orchards. If it is a wet season, it is even worse. Then there is the pruning and the mowing and raking and then praying for no early frost and no late rains. Wikipedia lists 43 fungal diseases of apples. Then there are the rusts, nematodes, viral diseases, and insects. These farmers need all the weapons they can get to hope to win this war year after year.
Oddly, the biggest cause of these problems is us consumers. We like to eat crisp shiny blemish-free apples in March long after the growing season. If we had suggested that to early apple growers like Thomas Jefferson or George Washington, they would have had a great laugh at our expense, and then taken another long draught of their hard apple cider. American consumers are very picky and these farmers can’t allow a single blemish from some fungus or an insect bite.
But let’s take more seriously two serious criticisms EWG makes of the USDA and the permitted use of these pesticides in the US. They are critical of the use of Diphenylamine in the post-harvest treatment of apples. They cite evidence that the amine group in the Diphenylamine may be converted to a carcinogen in the acidic conditions of the stomach and that its essentially cosmetic post-harvest use is not worth the risk. There is theoretical data for this but very little actual data on this possible effect. The Europeans with the Precautionary Principle have created a temporary threshold about 100-fold less than our EPA tolerance of 10 ppm. Based on the very picky esthetics of American consumers, I fully sympathize with growers who are trying to avoid every blemish as they hold fruit for the March and April markets. While the data show that 80% of samples had measurable levels, 20% had undetectable levels. I strongly suspect that even if the US dropped its tolerance to 1 ppm our growers would have little trouble meeting it. There is also the legal standard of De minimis. That is, does this issue really reach the bar of minimum legal threat? The highest single apple had a level of 3.8 ppm. If a person ate 10 lbs of apples with that level of Diphenylamine in a year and if a tenth of that converted to nitrosamine, that would be approximately 2 mg of carcinogen over a year, compared to all the healthy stuff that person got in those apples. I would hope that any reasonable judge would pronounce, “De minimis” and please spend my time with really important things like second-hand smoke in children.

The other concerning issue is the neonicotinoid insecticide Acetamiprid. These have indeed been of concern and may, just may, be one cause of the colony collapse disorder among honeybees. Insecticides are difficult to create and apply because they generally are broad spectrum and kill all kinds of bugs, including bees, which are one of our best valued insects. Acetamiprid is among the best of the neonicotinoids having about a tenth of the toxicity among bees as other classes of neonicotinoids. It also has a rather short half life once sprayed of about half an hour, compared to 2 hours for other neonicotinoids. The EPA tolerance is quite low at 1 ppm (about 0.2 mg in an average apple) and the insect war on apples is quite high. We need to allow these farmers some effective tools if we want apples at a reasonable price in our markets. There are alternative insecticides, but they are generally older, have known resistant species, and other known toxicities and side effects.
So, we have looked in some detail at the same data that EWG used for their assessment that apples perennially belong on the Dirty Dozen. Based on what we have seen, we seem to have remarkable safe apples grown by remarkably responsible growers. While there are always outliers and always more to learn about the chemicals we use, I think we can confidently say, “An apple a day (of almost any kind) keeps…” If all the other members of the Dirty Dozen are this dirty, then I declare them a Not Very Dirty Dozen and Paracelsus would agree.
In our next post we will come back to this. I will address the topics of analytical chemistry and the nutrition of the Dirty Dozen more fully next time.
My Credentials
I have recently become more conscious of the fact that we have too many printed opinions out there. One thing that we should do is limit our own printings to areas in which we are relative experts or in which we are relatively well read. To that end, here is why I feel qualified to address the deficiencies of the Dirty Dozen. This article is about pesticide residues in foods. I hold a BS in Biochemistry with several courses in Organic Chemistry. In fact, I am a member in good standing in the American Chemical Society. I have a MS in Environmental Toxicology with a course in Insecticide Toxicology. I have a PhD in Nutrition and my minor area was Analytical Chemistry. I also worked at a lab bench full time doing research for about 22 years. All that academic and research work was at Cornell University. I have since taught Nutrition courses at Appalachian State University from the introductory level (for which I am also the coauthor of a textbook) to the graduate level, including a graduate course in Statistics. I have also been doing research in epidemiology and also laboratory research on the phytochemical in apples. I have 30 peer-reviewed publications.